Mastitis
Discription of the disease
Mastitis is the most prevalent endemic disease afflicting dairy cattle. Mastitis
is the inflammation of the mammary gland and
udder tissue and usually can be indicated by an high somatic cell count (SCC) in
the milk. The SCC represents the number of cells per milliliter ml milk; the majority
consists of white blood cells and a small portion of epithelial cells. An
epithelial cell is a cell in the epithelium, the tissue that covers organs and
other tissues.
The white blood cells (leukocytes) play a major role in the immune system: they protect the body against various infections invaded by pathogens, such as bacteria and viruses, by detect and destroy them. So in fact, the SCC will increase after an inflammatory response (to pathogenic bacteria) in the mammary gland, due to an influx of white blood cells. The somatic cell count in the milk also increases after calving, when colostrum is produced.
The SCC is mentioned as ‘high’ in case of >200.000/ml in dairy cows and >150.000 in heifers. Even though milk with a high SCC most often indicates mastitis, this is not always visible; mastitis can either be clinical and subclinical. The last is not visible on the cow or her milk, this is only visible by the high SCC. Mostly, also a cow with clinical mastitis is not ill, but her milk looks abnormal (flakes). Clinical signs of acute mastitis include abnormal milk (watery with flakes); (red) swollen udder that is often painful; fever; lack of appetite and greatly reduced milk flow. Severe acute mastitis can be fatal to the cow.
There are a number of pathogenic micro-organisms that have the potential to cause mastitis. Mastitis is most often transmitted by contact with the milking machine, and through contaminated hands or other materials, in housing, bedding and other equipment.
The damage caused by mastitis is high for the effects of milk loss, cost of medication and vet visits, early discharge from cows and mastitis cows have fertility problems as well. (1,2,3,4)
The white blood cells (leukocytes) play a major role in the immune system: they protect the body against various infections invaded by pathogens, such as bacteria and viruses, by detect and destroy them. So in fact, the SCC will increase after an inflammatory response (to pathogenic bacteria) in the mammary gland, due to an influx of white blood cells. The somatic cell count in the milk also increases after calving, when colostrum is produced.
The SCC is mentioned as ‘high’ in case of >200.000/ml in dairy cows and >150.000 in heifers. Even though milk with a high SCC most often indicates mastitis, this is not always visible; mastitis can either be clinical and subclinical. The last is not visible on the cow or her milk, this is only visible by the high SCC. Mostly, also a cow with clinical mastitis is not ill, but her milk looks abnormal (flakes). Clinical signs of acute mastitis include abnormal milk (watery with flakes); (red) swollen udder that is often painful; fever; lack of appetite and greatly reduced milk flow. Severe acute mastitis can be fatal to the cow.
There are a number of pathogenic micro-organisms that have the potential to cause mastitis. Mastitis is most often transmitted by contact with the milking machine, and through contaminated hands or other materials, in housing, bedding and other equipment.
The damage caused by mastitis is high for the effects of milk loss, cost of medication and vet visits, early discharge from cows and mastitis cows have fertility problems as well. (1,2,3,4)
Cause
Besides some more rare causes such as viruses, mycoplasma and yeast/fungi, mastitis is the response to an invasion of bacteria to the teat canal. The main causes in mastitis are three groups of bacteria: coli form species, streptococci and staphylococci. Those bacteria damage the milk-secreting tissue as well as various ducts throughout the mammary gland by toxins. Each group of these bacteria has other specific properties and a corresponding plan of action. By residual bacteria in the milking machine, pathogens are transferred easily from cow-to-cow, since most common mastitis pathogens are found in the udder tissues.
The mastitis pathogens can be classified as either infectious or non-infectious. The non-infectious can be classified as either environmental or opportunistic. Opportunism refers to the ability of a normally non-pathogenic microorganism to act as a pathogen in certain circumstances. Opportunist bacteria are ones that take advantage of certain situations; when those bacteria invade the host organism it can cause infection in the host organism, but cause real disease only if the natural defenses, resistance or immune system of the host organism are lowered by certain reasons. This is why it is important to know the risk factors.
A cow is particularly susceptible for getting an infection when unfavorable conditions for the cows, which are beneficial for the bacteria, occur. (5,6)
The mastitis pathogens can be classified as either infectious or non-infectious. The non-infectious can be classified as either environmental or opportunistic. Opportunism refers to the ability of a normally non-pathogenic microorganism to act as a pathogen in certain circumstances. Opportunist bacteria are ones that take advantage of certain situations; when those bacteria invade the host organism it can cause infection in the host organism, but cause real disease only if the natural defenses, resistance or immune system of the host organism are lowered by certain reasons. This is why it is important to know the risk factors.
A cow is particularly susceptible for getting an infection when unfavorable conditions for the cows, which are beneficial for the bacteria, occur. (5,6)
Pathogenesis
Contagious
pathogens tend to live on the udder and teat skin of the cow, mainly
transferred during milking or lying down in leaked milk from an infected cow.
Mastitis pathogens can also be present in the environment such as the housing
and bedding. These pathogens can be transferred during milking as well as
during the rest of the cow’s pastimes like lying down, walking and eating.
Environmental pathogens in general are not able to settle in the teat, so dry
cow therapy has little value to get rid of these infections in the (next)
lactation: the udder does not carry them to that.
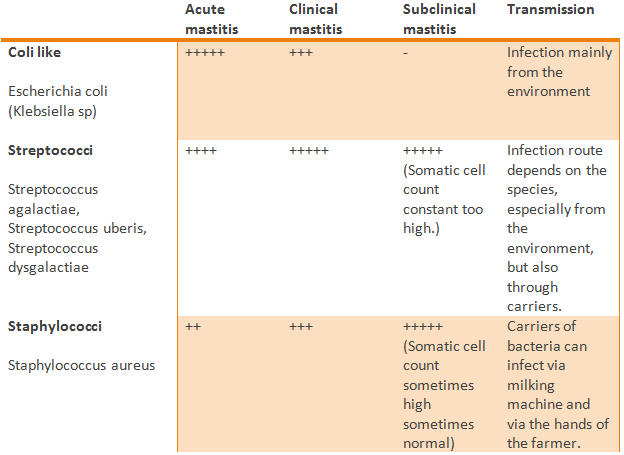
The table below shows the major pathogens causing (different states of) mastitis:
The table below shows the major pathogens causing (different states of) mastitis:
The
contagious mastitis bacteria of greatest concern are the Staphylococcus aureus
(coagulate-positive) and Streptococcus
agalactiae. The environmental mastitis pathogens of greatest concern are
the coliforms: Eschericia coli and Klebsiella sp.; and the
environmental streptococci, Streptococcus uberis and dysgalactiae. The primary Mycoplasma species, M.
bovis and M. Californicum, are
causing mastitis less commonly.
The opportunistic pathogens are the coagulase-negative staphylococci (staphylococcus aureus). Coagulase, an exo-enzym, has the ability to coagulate blood plasma, which is distinctive for the contagious Staphyloccocus aureus. This enzym is able to convert fibrinogen in bloodplasma to fibrin whereby it is visible on the microscope slide. (5,2)
Escherichia coli
Escherichia coli is a gram-negative rod-shaped bacterium and is one of the most common facultative anaerobic bacteria in the large intestines of warm-blooded animals, such as mammals and is required for the digestion of food. This Enterobacteriaceae is often used as model for bacteria in general.
E. coli and other coli-form bacteria (called ECO) are located in the vicinity of the cow (manure, boxes, bottom). Coli-form bacteria are bacteria that are more or less behave like E.coli and approximately the same properties and the same environmental complexity. Coli-forms include Enterobacteria, Citrobacteria, and Serratia. Klebsiella can be charged up too.
E. coli usually causes clinical mastitis with a hard, swollen udder and watery milk. Milk samples from suspected E.coli mastitis cases are quite often tested negative. The bacterium has disappeared at the moment of sampling, because the cow is ill of the poison (toxin) which comes from the bacterium itself, at the time that the bacteria will die. (7,8)
Streptococci
Bacteria that have the potential to cause mastitis include Streptococcus agalactiae, Streptococcus dysgalactiae and Streptococcus uberis.
The streptococci (Streptococcus) are a species of bacteria from Gram-positive, facultatively anaerobic cocci. Cell division occurs along a single axis in this bacterial genus. As a result, they grow in a chain form or as pairs, hence the name derived from the Greek streptos what turned or easily bendable means (such as a necklace).
Streptococci are both useful and pathogenic bacteria to humans and animals. They are mainly found in the in the nasal cavity, in the pharynx and on the skin, which manifests a possible infection. ¹,9
Staphylococci
The genus Staphylococcus are bacteria belonging to the family Staphylococcaceae. The colonies are round and have a white to golden yellow pigment. The genus has about 20 species; on dairy farms with high SCC problems due to subclinical mastitis often Staph. aureus is demonstrated as the most important pathogen. This bacterium is immobile, catalase-positive, oxidase-negative and grows facultative anaerobic. Most strains of Staphylococcus aureus are contagious: this means that these bacteria need the cow’s udder, skin, mouth, vagina and/or milk to survive and multiply. The aureus bacteria are located on the udder of the cow, but also in the milk; aureus infection occurs mainly via the milking machine. These cows are cows are a major source of infection to other cows.
Some strains within the group of bacteria Staphylococcus aureus bacteria behave more like environmental/opportunistic bacteria.
Cows with subclinical mastitis caused by Staphylococcus aureus, increase SCC in bulk tank. However, the number of bacteria that are excreted in the milk can fluctuate; thereby the SCC changes often. It is difficult to demonstrate the presence of Staphulococcus aureus since it has the ability to enhold itself in a mucus layer (biofilm), to form little abscesses or to encapsulate in (higher) udder tissues. This means that the bacterium is able to shield for the immune system and to survive, because they will no longer be recognized by the defence cells of the cow.
Bacteriological examination on aureus will often give a false-negative result, due to the characteristics named above, but following samples (2-3 times) will increase the sensitivity of the examination to 94-98%.
Because of the increased problems in human health related to the MRSA (Meticilline Resistent Staphylococcus Aureus) bacteria and antibiotic use has an impact on both animal health, human health and the environmental health, which make it important to search for alternatives to antibiotics and preventive measures. (10,11)
The opportunistic pathogens are the coagulase-negative staphylococci (staphylococcus aureus). Coagulase, an exo-enzym, has the ability to coagulate blood plasma, which is distinctive for the contagious Staphyloccocus aureus. This enzym is able to convert fibrinogen in bloodplasma to fibrin whereby it is visible on the microscope slide. (5,2)
Escherichia coli
Escherichia coli is a gram-negative rod-shaped bacterium and is one of the most common facultative anaerobic bacteria in the large intestines of warm-blooded animals, such as mammals and is required for the digestion of food. This Enterobacteriaceae is often used as model for bacteria in general.
E. coli and other coli-form bacteria (called ECO) are located in the vicinity of the cow (manure, boxes, bottom). Coli-form bacteria are bacteria that are more or less behave like E.coli and approximately the same properties and the same environmental complexity. Coli-forms include Enterobacteria, Citrobacteria, and Serratia. Klebsiella can be charged up too.
E. coli usually causes clinical mastitis with a hard, swollen udder and watery milk. Milk samples from suspected E.coli mastitis cases are quite often tested negative. The bacterium has disappeared at the moment of sampling, because the cow is ill of the poison (toxin) which comes from the bacterium itself, at the time that the bacteria will die. (7,8)
Streptococci
Bacteria that have the potential to cause mastitis include Streptococcus agalactiae, Streptococcus dysgalactiae and Streptococcus uberis.
The streptococci (Streptococcus) are a species of bacteria from Gram-positive, facultatively anaerobic cocci. Cell division occurs along a single axis in this bacterial genus. As a result, they grow in a chain form or as pairs, hence the name derived from the Greek streptos what turned or easily bendable means (such as a necklace).
Streptococci are both useful and pathogenic bacteria to humans and animals. They are mainly found in the in the nasal cavity, in the pharynx and on the skin, which manifests a possible infection. ¹,9
Staphylococci
The genus Staphylococcus are bacteria belonging to the family Staphylococcaceae. The colonies are round and have a white to golden yellow pigment. The genus has about 20 species; on dairy farms with high SCC problems due to subclinical mastitis often Staph. aureus is demonstrated as the most important pathogen. This bacterium is immobile, catalase-positive, oxidase-negative and grows facultative anaerobic. Most strains of Staphylococcus aureus are contagious: this means that these bacteria need the cow’s udder, skin, mouth, vagina and/or milk to survive and multiply. The aureus bacteria are located on the udder of the cow, but also in the milk; aureus infection occurs mainly via the milking machine. These cows are cows are a major source of infection to other cows.
Some strains within the group of bacteria Staphylococcus aureus bacteria behave more like environmental/opportunistic bacteria.
Cows with subclinical mastitis caused by Staphylococcus aureus, increase SCC in bulk tank. However, the number of bacteria that are excreted in the milk can fluctuate; thereby the SCC changes often. It is difficult to demonstrate the presence of Staphulococcus aureus since it has the ability to enhold itself in a mucus layer (biofilm), to form little abscesses or to encapsulate in (higher) udder tissues. This means that the bacterium is able to shield for the immune system and to survive, because they will no longer be recognized by the defence cells of the cow.
Bacteriological examination on aureus will often give a false-negative result, due to the characteristics named above, but following samples (2-3 times) will increase the sensitivity of the examination to 94-98%.
Because of the increased problems in human health related to the MRSA (Meticilline Resistent Staphylococcus Aureus) bacteria and antibiotic use has an impact on both animal health, human health and the environmental health, which make it important to search for alternatives to antibiotics and preventive measures. (10,11)
Diagnosis
In many problems with increased cell count in the business, it is handy to do bacteriological examination to address the exact type of bacteria.
Subclinical mastitis can be up to 40 times more common than clinical cases of the illness.
Symptoms in clinical mastitis are visible for the farmer; this makes it easier for the farmer to detect clinical mastitis in the herd. The degree of severity in clinical mastitis can range from mild to moderate to severe; dependent on for example the nutritional or immune status of the cow, involved pathogens, environmental factors like hygiene, humidity and ambient.
Clinical mastitis can either be acute or chronic, the subclinical state of mastitis is chronic most of time. This terms indicate how long the disease lasts and how quickly it develops, not the severity of the disease. In the acute form the disease comes up relatively suddenly in a formerly healthy cow. The severity can be divided into per-acute referring to severe inflammations or sub-acute for milder inflammations.
Long-termed cases of mastitis are named chronic, these cases keep recurring. (12,13)
Subclinical mastitis can be up to 40 times more common than clinical cases of the illness.
Symptoms in clinical mastitis are visible for the farmer; this makes it easier for the farmer to detect clinical mastitis in the herd. The degree of severity in clinical mastitis can range from mild to moderate to severe; dependent on for example the nutritional or immune status of the cow, involved pathogens, environmental factors like hygiene, humidity and ambient.
Clinical mastitis can either be acute or chronic, the subclinical state of mastitis is chronic most of time. This terms indicate how long the disease lasts and how quickly it develops, not the severity of the disease. In the acute form the disease comes up relatively suddenly in a formerly healthy cow. The severity can be divided into per-acute referring to severe inflammations or sub-acute for milder inflammations.
Long-termed cases of mastitis are named chronic, these cases keep recurring. (12,13)
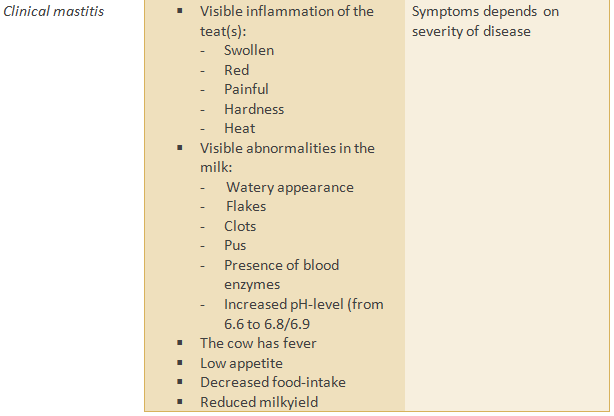
Symptoms
The degree of
severity in clinical mastitis can range from mild to moderate to severe;
dependent on for example the nutritional or immune status of the cow, involved
pathogens, environmental factors like hygiene, humidity and ambient.
|
Mild mastitis
|
Sick cow with mastitis
|
Severe sick cow with
mastitis
|
Consequences
Consequences of mastitis will depend on the state, the severity and the involved pathogens.
Compositional milk changes
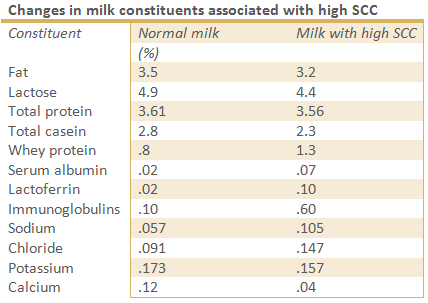
The major pathogens in mastitis (named in the paragraph ‘pathogens’) are causing changes in composition of milk which reduces the milkquality, both in cows suffering from subclinical- and clinical mastitis.
The overall milkprotein content may be unaffected, the types of milkproteins change; casein, an important, high quality protein found in healthy milk, can be reduced in cows suffering from subclinical mastitis by entering of low-quality blood serum proteins (e.g. serum albumin, immunoglobulins, transferring) into milk because the changes in vascular permeability.
An other complication is that calcium level in the milk is lowered as well in casein synthesis, since most calcium in milk is closely linked with casein levels in milk production.
Milk protein breakdown can occur in milk from cows with clinical or subclinical mastitis when proteolytic enzymes are presented. During mastitis, plasmine, an enzym in blood, doubles the proteolytic activity. Plasmines and other enzymes originating from white bloodcells, can cause damage casein in the udder (before milking); this deterioration of milk protein may continue during processing and storage of the milk. The presence of certain blood enzymes can influence the taste of milk negatively, as well as the possibility of processing the milk into cheese or yogurt.
Sodium and chloride concentrations increase; and level of potassium, normally the main mineral in milk, decreases.
Chemical changes in the milk can result in an increased pH level; where the normal acidity of milk is about 6.6, the pH level of milk can rise to 6.8/6.9 in cows with mastitis. (13,14)
The major pathogens in mastitis (named in the paragraph ‘pathogens’) are causing changes in composition of milk which reduces the milkquality, both in cows suffering from subclinical- and clinical mastitis.
The overall milkprotein content may be unaffected, the types of milkproteins change; casein, an important, high quality protein found in healthy milk, can be reduced in cows suffering from subclinical mastitis by entering of low-quality blood serum proteins (e.g. serum albumin, immunoglobulins, transferring) into milk because the changes in vascular permeability.
An other complication is that calcium level in the milk is lowered as well in casein synthesis, since most calcium in milk is closely linked with casein levels in milk production.
Milk protein breakdown can occur in milk from cows with clinical or subclinical mastitis when proteolytic enzymes are presented. During mastitis, plasmine, an enzym in blood, doubles the proteolytic activity. Plasmines and other enzymes originating from white bloodcells, can cause damage casein in the udder (before milking); this deterioration of milk protein may continue during processing and storage of the milk. The presence of certain blood enzymes can influence the taste of milk negatively, as well as the possibility of processing the milk into cheese or yogurt.
Sodium and chloride concentrations increase; and level of potassium, normally the main mineral in milk, decreases.
Chemical changes in the milk can result in an increased pH level; where the normal acidity of milk is about 6.6, the pH level of milk can rise to 6.8/6.9 in cows with mastitis. (13,14)
Performance
Losses in milkyield can occur, Prof. Dr. Vliegher de Sarna stated in 2012: “Infected cows do not produce quite optimal; cows with subclinical mastitis caused by Staphylococcus aureus produce 1.5 kg (heifers) to 2.0 kg (adult cow) less milk per day than they could with a healthy udder.” Of course this depends on the severity of inflammation.
Fertility disorders in mastitic cows are mostly connected with the activity of cytokines (especially TNF-alpha, which stimulates the inflammatory response in the body); cortisol, an stress hormone; prostaglandin F2-alpha, produced by the uterus of domestic mammals when stimulated by oxytocin and stops the production of progesterone by the corpus luteum; and inflammatory mediators; responsible for the clinical signs of inflammation. (15,16)
Economic
Mastitis results in several economical losses, such as:
Mastitis results in several economical losses, such as:
- Throw away milk due to contamination by medication or the milk-quality is too low, which makes it unfit to process
- A reduction in yields due to illness and any permanent damage to udder tissue.
- The extra labour which is required for treating the infected animals
- Veterinary costs; extra visits and medication
- The cost of reduced longevity due to premature culling
- Decreased milk yield (4)
List of sources
1.
Hunter, F. (2004) Everyday homeopathy for animals,
Beaconsfield: Beaconsfield Publishers LTD.
2. D.A.P. Bladel-Hapert (2014) Uierontsteking bij koeien. Available at: < http://www.dapbladelhapert.nl/mastitis.htm > [Accessed 05 June 2014].
3. Handboek uiergezondheid (2014) Celgetal - Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Celgetal.> [Accessed 05 June 2014].
4. (2014) Mastitis in dairy cows. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/#.U5Y6QfnV9Fs >. [Accessed 05 June 2014].
5. Lawrence, K. Fox () Mastitis control: the basics. College of veterinary medicine – Washington State University.
6. ( 2014) Opportunism - Wikipedia. Available at: <http://en.wikipedia.org/wiki/Opportunism#Biological_opportunism. > [Accessed 05 June 2014]
7. Handboek Uiergezondheid (2014) Behandelen: Escherichia coli. Available at: < http://www.handboekuiergezondheid.nl/behandelen/specifiekemastitisverwekkers/escheriacoli > [Accessed 05 June 2014].
8. (2014) Escherichia coli – Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Escherichia_coli.> [Accessed 05 June 2014]
9. (2014) Streptokokken - Wikipedia. Available at: <http://nl.wikipedia.org/wiki/Streptokokken>. [Accessed 05 June 2014]
10. Handboek Uiergezondheid (2014) Behandelen: Staphylococcus aureus. Available at: <http://www.handboekuiergezondheid.nl/behandelen/specifiekemastitisverwekkers/staphylococcusaureus> [Accessed 05 June 2014]
11. (2014) Stafylokokken - Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Stafylokokken. >[Accessed 05 June 2014]
12. (2014) Sub-clinical mastitis. Available at: <http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/symptoms-of-mastitis/sub-clinical-mastitis/#.U5WzvPnV9Fs> [Accessed 05 June 2014]
13. (2014) Symptoms of Mastitis. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/symptoms-of-mastitis/#.U5W4rPnV9Fs>. [Accessed 05 June 2014].
14. Jones, G.M., (2009) Understanding the basics of mastitis. Virginia-Maryland College of Veterinary Medicine, Virginia Tech. Available from: < http://pubs.ext.vt.edu/404/404-233/404-233.html> [Accessed 05 June 2014]
15. Malinowski, E., Gajewski, Z., (2010) Mastitis and fertility disorders in cows. Available from: < http://www.ncbi.nlm.nih.gov/pubmed/21033574> [Accessed 05 June 2014]
16. Seegers, H., Fourichon, C., Beaudeau, F. (2003) Production effects related to mastitis and mastitis economics in dairy cattle herds. Unit of Animal Health Management, National Veterinary School, France. Available from: < http://hal.archives-ouvertes.fr/docs/00/90/27/68/PDF/hal-00902768.pdf > [Accessed 05 June 2014]
17. UGCN. (-). Mastitis. Available: http://www.ugcn.nl/media/default.aspx/emma/org/10647926/samenvatting%20bart%20van%20der%20borne.pdf. [Accessed 05 June 2014]
18. (2014) Pathogens - The cause of mastitis. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/pathogens-the-cause-of-mastitis/#.U5WTdvnV9Fs >. [Accessed 05 June 2014].
19. Levende have. (2013). Mastitis. Available: < http://www.levendehave.nl/kennisbank/runderen/mastitis> [Accessed 05 June 2014]
20. Groot M., Kleijer-Ligtenberg, G., van Asseldonk T., Hansma, H., [2011] Stalboekje Melkvee – Natuurlijk gezond met kruiden en andere natuurproducten. Available from: <http://edepot.wur.nl/162983> [24 May 2014]
21. Finke, E. (2011) Bedrijfsnetwerk op weg naar minder antibiotica. Available from: < http://edepot.wur.nl/185222> [24 May 2014]
22. Ryckaert, I. (-) Levensproductie van melkkoeien. Vlaamse overheid, Departement Landbouw en Visserij, Afdeling Duurzame Landbouwontwikkeling. Available from: < http://www2.vlaanderen.be/landbouw/downloads/dier/22.pdf> [Accessed 05 June 2014]
23. Deru, J., Ellinger, L., Baars, T., [2006] Homeopathie bij rundvee een verkenning van behandelingen, succesfactoren en patroonherkenning in het kader van Bioveem – Bioveem Intern Rapport 16. Available from: http://www.centaurea.nl/wp-content/uploads/2010/04/Homeopathie-bij-rundvee.pdf [24 May 2014]
24. Werkgroep Veterinair Antibiotica Beleid – KNMVD [2012] Formularia antibiotica from: <http://wvab.knmvd.nl/wvab/formularia/formularia> [24 May 2014]
25. (-). Mastitis in dairy cattle – Wikipedia. Available at: < http://en.wikipedia.org/wiki/Mastitis_in_dairy_cattle.> [Accessed 05 June 2014]
2. D.A.P. Bladel-Hapert (2014) Uierontsteking bij koeien. Available at: < http://www.dapbladelhapert.nl/mastitis.htm > [Accessed 05 June 2014].
3. Handboek uiergezondheid (2014) Celgetal - Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Celgetal.> [Accessed 05 June 2014].
4. (2014) Mastitis in dairy cows. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/#.U5Y6QfnV9Fs >. [Accessed 05 June 2014].
5. Lawrence, K. Fox () Mastitis control: the basics. College of veterinary medicine – Washington State University.
6. ( 2014) Opportunism - Wikipedia. Available at: <http://en.wikipedia.org/wiki/Opportunism#Biological_opportunism. > [Accessed 05 June 2014]
7. Handboek Uiergezondheid (2014) Behandelen: Escherichia coli. Available at: < http://www.handboekuiergezondheid.nl/behandelen/specifiekemastitisverwekkers/escheriacoli > [Accessed 05 June 2014].
8. (2014) Escherichia coli – Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Escherichia_coli.> [Accessed 05 June 2014]
9. (2014) Streptokokken - Wikipedia. Available at: <http://nl.wikipedia.org/wiki/Streptokokken>. [Accessed 05 June 2014]
10. Handboek Uiergezondheid (2014) Behandelen: Staphylococcus aureus. Available at: <http://www.handboekuiergezondheid.nl/behandelen/specifiekemastitisverwekkers/staphylococcusaureus> [Accessed 05 June 2014]
11. (2014) Stafylokokken - Wikipedia. Available at: < http://nl.wikipedia.org/wiki/Stafylokokken. >[Accessed 05 June 2014]
12. (2014) Sub-clinical mastitis. Available at: <http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/symptoms-of-mastitis/sub-clinical-mastitis/#.U5WzvPnV9Fs> [Accessed 05 June 2014]
13. (2014) Symptoms of Mastitis. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/symptoms-of-mastitis/#.U5W4rPnV9Fs>. [Accessed 05 June 2014].
14. Jones, G.M., (2009) Understanding the basics of mastitis. Virginia-Maryland College of Veterinary Medicine, Virginia Tech. Available from: < http://pubs.ext.vt.edu/404/404-233/404-233.html> [Accessed 05 June 2014]
15. Malinowski, E., Gajewski, Z., (2010) Mastitis and fertility disorders in cows. Available from: < http://www.ncbi.nlm.nih.gov/pubmed/21033574> [Accessed 05 June 2014]
16. Seegers, H., Fourichon, C., Beaudeau, F. (2003) Production effects related to mastitis and mastitis economics in dairy cattle herds. Unit of Animal Health Management, National Veterinary School, France. Available from: < http://hal.archives-ouvertes.fr/docs/00/90/27/68/PDF/hal-00902768.pdf > [Accessed 05 June 2014]
17. UGCN. (-). Mastitis. Available: http://www.ugcn.nl/media/default.aspx/emma/org/10647926/samenvatting%20bart%20van%20der%20borne.pdf. [Accessed 05 June 2014]
18. (2014) Pathogens - The cause of mastitis. Available at: < http://www.dairyco.org.uk/technical-information/animal-health-welfare/mastitis/pathogens-the-cause-of-mastitis/#.U5WTdvnV9Fs >. [Accessed 05 June 2014].
19. Levende have. (2013). Mastitis. Available: < http://www.levendehave.nl/kennisbank/runderen/mastitis> [Accessed 05 June 2014]
20. Groot M., Kleijer-Ligtenberg, G., van Asseldonk T., Hansma, H., [2011] Stalboekje Melkvee – Natuurlijk gezond met kruiden en andere natuurproducten. Available from: <http://edepot.wur.nl/162983> [24 May 2014]
21. Finke, E. (2011) Bedrijfsnetwerk op weg naar minder antibiotica. Available from: < http://edepot.wur.nl/185222> [24 May 2014]
22. Ryckaert, I. (-) Levensproductie van melkkoeien. Vlaamse overheid, Departement Landbouw en Visserij, Afdeling Duurzame Landbouwontwikkeling. Available from: < http://www2.vlaanderen.be/landbouw/downloads/dier/22.pdf> [Accessed 05 June 2014]
23. Deru, J., Ellinger, L., Baars, T., [2006] Homeopathie bij rundvee een verkenning van behandelingen, succesfactoren en patroonherkenning in het kader van Bioveem – Bioveem Intern Rapport 16. Available from: http://www.centaurea.nl/wp-content/uploads/2010/04/Homeopathie-bij-rundvee.pdf [24 May 2014]
24. Werkgroep Veterinair Antibiotica Beleid – KNMVD [2012] Formularia antibiotica from: <http://wvab.knmvd.nl/wvab/formularia/formularia> [24 May 2014]
25. (-). Mastitis in dairy cattle – Wikipedia. Available at: < http://en.wikipedia.org/wiki/Mastitis_in_dairy_cattle.> [Accessed 05 June 2014]